
10 Behavioral Health Assessments to Identify Patient Needs
Misdiagnosis is a common reality for patients with mental...
Read article
Evaluate symptoms of Post-Traumatic Stress Disorder (PTSD) quickly and reliably with a digitized version of the PCL-5 questionnaire. Quantify test for PTSD symptoms, quantify symptom severity, and support PTSD diagnosis, monitoring, and treatment decisions, according to DSM-5 criteria.


The PCL-5 is a self-report PTSD checklist developed by the National Center for PTSD to align with DSM-5 criteria. It helps identify a provisional PTSD diagnosis, monitor symptom change, and assess treatment effectiveness.
Backed by strong psychometric properties—including internal consistency and test-retest reliability—the PCL-5 provides both a total symptom severity score and cluster severity scores, supporting accurate diagnosis and tracking of clinically significant change.
Post-traumatic stress disorder can be difficult to recognize—especially when symptoms overlap with other conditions. The PCL-5 helps bring structure and clarity to the evaluation process, giving clinicians a consistent way to assess symptom presence, severity, and impact.

The PCL-5 offers a standardized format for evaluating PTSD symptoms across patients and settings, helping ensure no key criteria are overlooked and that assessments are guided by DSM-5 guidelines for diagnosing PTSD.

Built on strong psychometric evidence—including internal consistency and test-retest reliability—the PCL-5 provides symptom severity and cluster scores that support accurate, defensible diagnostic decisions.

Total and cluster symptom severity scores help clinicians monitor patient progress and detect clinically significant change--evaluating treatment effectiveness and ensuring care plans adapt based on measurable outcomes.
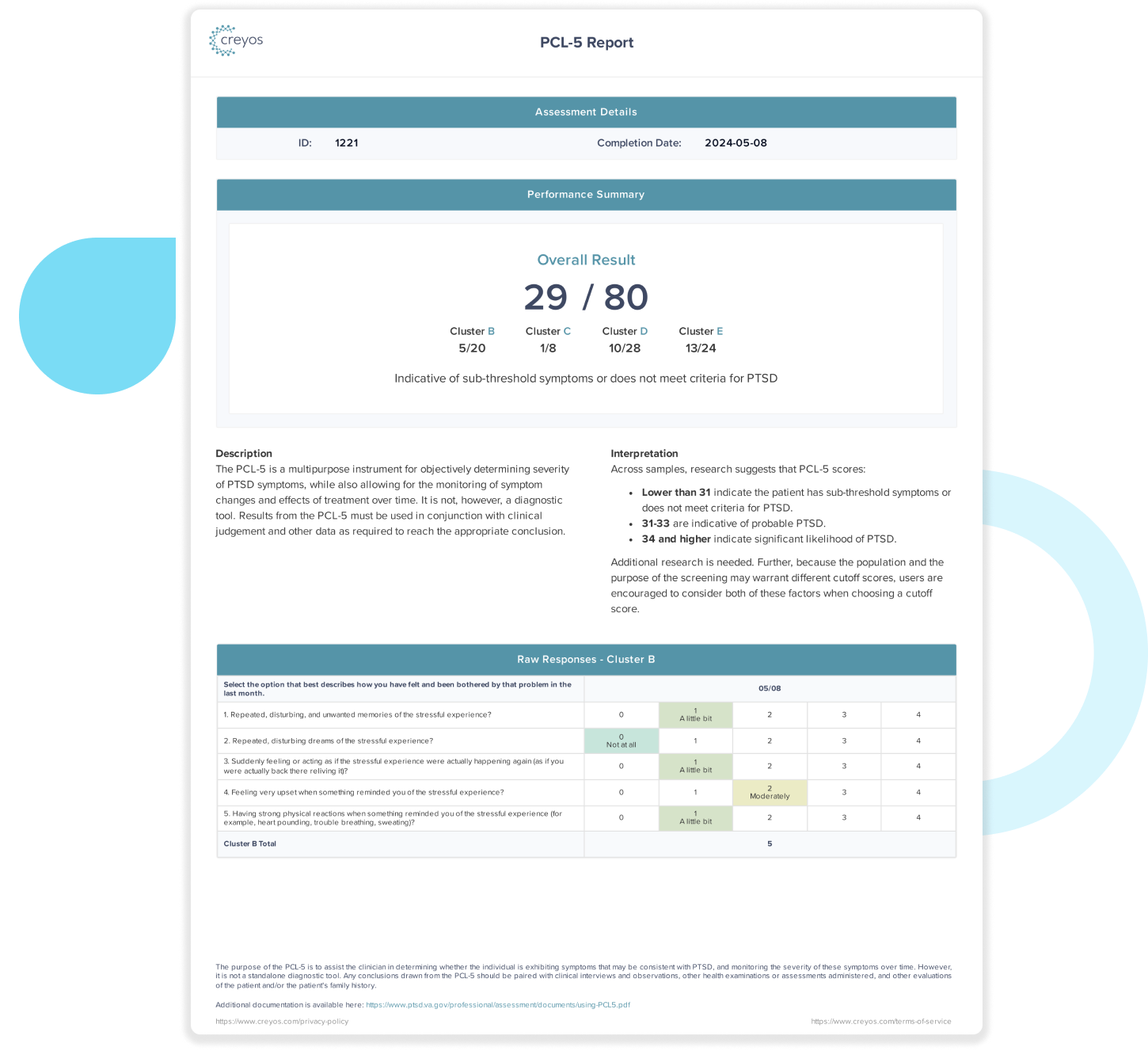
The PCL-5 questionnaire in Creyos is a 20-question self-assessment that measures a patient's PTSD symptoms. It helps clinicians make informed decisions about PTSD diagnosis, treatment, and follow-up—without added complexity.
Efficient, digital, and clinically grounded—Creyos makes it easier to monitor and manage post traumatic stress disorder in any setting.







Experiencing or witnessing a traumatic event can have a profound and long-lasting impact on a person’s life, and the World Health Organization estimates that nearly 4% of the global population has experienced PTSD at some point in their lives. This condition can significantly affect cognitive health, causing difficulties with concentration, memory, emotional processing, and executive functioning. Understanding PTSD symptoms is the key to treatment, and the PCL-5 in Creyos Health can help.
Source: World Health Organization, 2024

Administer the PTSD Checklist for DSM-5 (PCL-5) alongside other behavioral health questionnaires and cognitive tests—all in one platform that’s easy for both clinicians and patients to use. No juggling systems, no manual scoring—just a streamlined way to assess symptoms, track changes, and support better mental health care.

The PCL-5 demonstrates strong internal consistency and test-retest reliability, with initial psychometric evaluations confirming its discriminant validity. Developed by the National Center for PTSD, the tool is supported by research from the Behavioral Science Division and is considered a reliable instrument for identifying clinically meaningful change in PTSD symptom severity over time.
When a patient completes the PCL-5 checklist, providers get immediate insights through easy-to-read reports that combine questionnaire data with cognitive test results for a full picture of patient brain health. Creyos integrates with dozens of EHRs through APIs and built-in integrations with AdvancedMD, athenahealth, and Epic. Our platform automatically collects, scores, and organizes results from each questionnaire and adds them to the patient’s record in your EHR.
No, while the PCL-5 is a valuable tool for screening and tracking PTSD symptoms, a formal PTSD diagnosis should be made using a structured clinical interview and other inputs. The PCL-5 questionnaire helps clinicians gather information quickly, but it is not intended to replace a comprehensive clinical assessment or be the sole tool used in diagnosis.
Because it is a repeatable item self-report measure, the PCL-5 allows clinicians to monitor symptom change over time. By comparing symptom severity scores across sessions, providers can evaluate treatment effectiveness, identify clinically significant change, and adjust care plans accordingly. It is especially useful in long-term care and trauma-informed treatment settings.
The PTSD checklist for DSM-5 includes symptoms such as unwanted memories, difficulty concentrating, angry outbursts, irritable behavior, strong negative beliefs, trouble experiencing positive feelings, and strong physical reactions to trauma-related cues. These symptoms are aligned with the DSM-5 PTSD criteria, specifically Clusters B (intrusion), C (avoidance), D (negative alterations in cognition and mood), and E (arousal and reactivity).

Misdiagnosis is a common reality for patients with mental...
Read article

Among mental health concerns in the general population,...
Read article

About half of those who experience a mental illness during...
Read article